Atelectasis
Partial collapse or incomplete expansion of lung tissue
Atelectasis means part of the lung is not expanding fully and often appears as opacity combined with signs of volume loss on X-ray.
Atelectasis means part of the lung has partially collapsed or is not inflating normally. It often appears after shallow breathing, obstruction, or pressure from outside the lung.
Representative X-ray
Illustrative reference image for this topic.
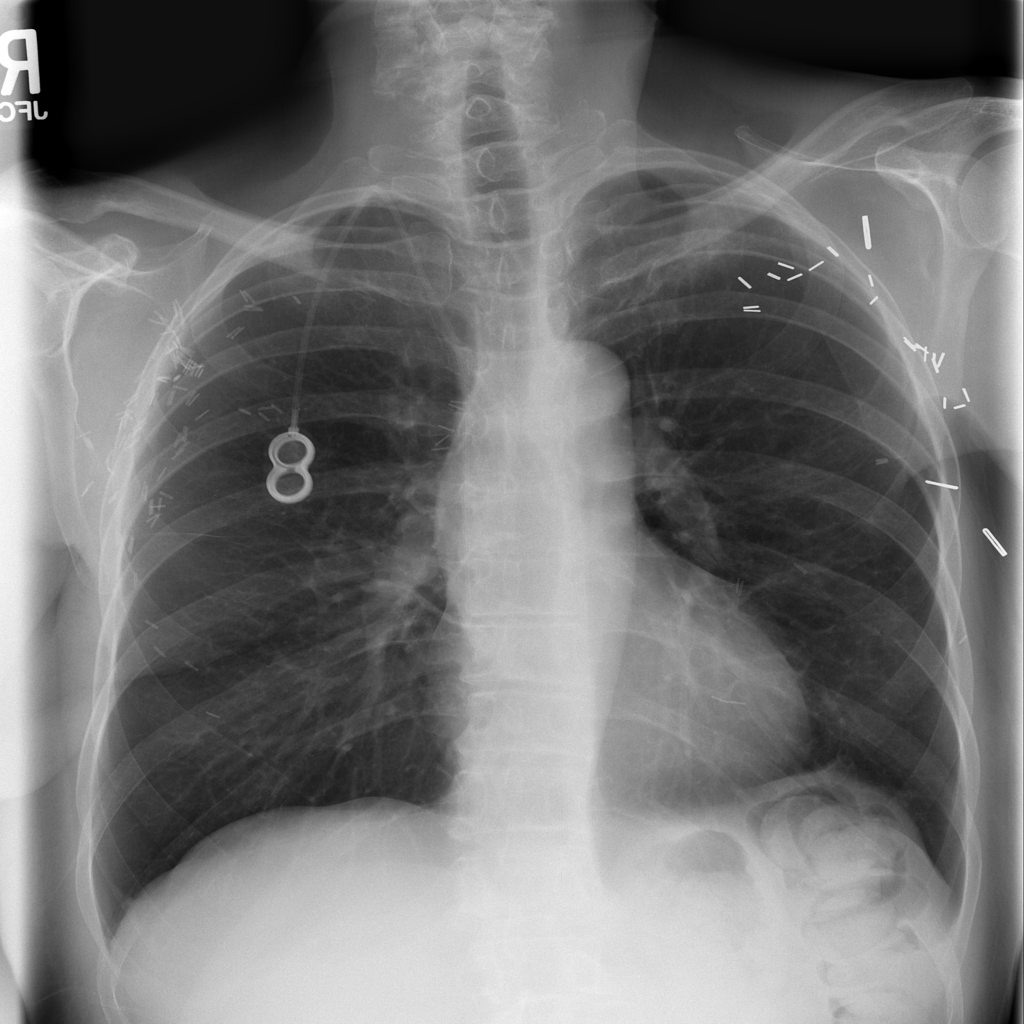
Reference image: PAT-69E4 · IMG-000 · Bounding-box highlight from source annotation where available.
What it is
- Atelectasis is loss of normal air volume in part of the lung
- It is a radiographic finding that can arise from airway obstruction, compression, low ventilation, postoperative change, or adjacent pleural disease
How it appears on chest X-ray
- On chest X-ray, atelectasis often appears as increased opacity plus signs of volume loss such as fissure shift, diaphragmatic elevation, crowding of vessels, or displacement of nearby structures
What radiologists look for
- Radiologists look for volume loss, shifted fissures, elevated hemidiaphragm, crowding of bronchi or vessels, and whether an obstructing lesion or pleural process could explain the change
How X-ray helps
- Chest X-ray can show both the denser area and the volume-loss clues that make atelectasis different from some other causes of opacity, although CT may be needed in selected cases
Common causes
- Common causes include postoperative shallow breathing, mucus plugging, airway obstruction, compression from pleural effusion, and low lung-volume states
Symptoms / associated symptoms
- Symptoms vary with extent and cause
- Some patients have cough or shortness of breath, while small areas of atelectasis may be clinically subtle
Risk factors
- Risk factors can include recent surgery, immobility, sedation, poor cough, airway obstruction, and underlying lung disease
Why it can matter clinically
- Atelectatic lung can reduce gas exchange and may coexist with infection, secretion retention, or underlying obstructive pathology
When to seek medical care
- Breathing difficulty, persistent postoperative shortness of breath, fever, or concern for airway obstruction should prompt medical review
Evaluation and diagnosis
- Evaluation may include chest imaging, assessment of recent surgery or illness, oxygen status, and investigation for obstruction or associated pleural disease when indicated
Treatment approaches
- Management depends on cause
- Treatment may include pulmonary hygiene, mobilization, pain control, breathing exercises, airway clearance, and addressing obstruction or pleural compression
Medication classes clinicians may use
Medication use depends on the cause and symptoms. In some cases, bronchodilator therapy, pain control, or cause-directed treatment may be relevant.
Treatment modalities commonly paired with medication decisions
- breathing exercises
- mobilization
- pulmonary hygiene
- airway clearance
- treating the underlying cause
Pain relievers
Can matter after surgery when pain limits deep breathing and lung expansion.
- acetaminophen
- ibuprofen
Bronchodilator therapy in selected settings
May help when bronchospasm or underlying obstructive lung disease contributes to poor ventilation.
- albuterol
Need help reviewing your own X-ray?
If you landed here because you are trying to understand a chest X-ray result, you can upload an image for an educational review and then use the related finding guides to go deeper.
FAQ
Is atelectasis the same as pneumonia?
No. They can both create opacity on imaging, but atelectasis is primarily volume loss while pneumonia is infection of lung tissue.
Can small atelectatic changes happen after surgery?
Yes. Mild postoperative atelectatic change is common, especially when breathing is shallow.